A University of Glasgow scientist is set to play a leading role in a ground breaking clinical trial for people with lung cancer.

Professor Anthony Chalmers, from the University’s Institute of Cancer Sciences, is one of a group of scientists from across the UK awarded £900,000 from Cancer Research UK to launch the CONCORDE trial.
The trial will explore the use of a number of new drugs alongside standard radiotherapy in the hope of improving survival for people with advanced non-small cell lung cancer.
Lung cancer is the most common cancer in Scotland, with around 5,300 people diagnosed each year*. Around 80 – 85% of lung cancers in the UK are non small cell lung cancer (NSCLC)**, which start in the mucus making gland cells in the lining of the airways.
Approximately 25% of NSCLC lung cancer patients are diagnosed with stage 3 disease, meaning that the cancer has spread from where it started to nearby tissue or lymph nodes.
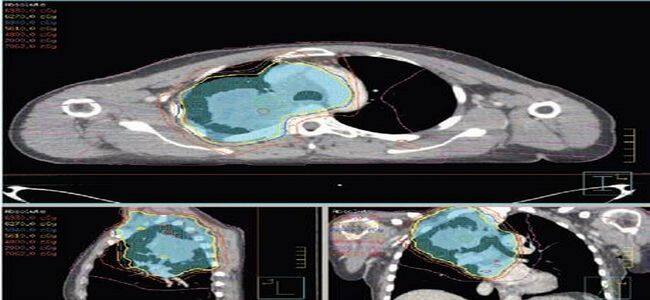
Radiotherapy is an important component of treatment in patients with this stage of NSCLC, and although it can successfully treat about half of these patients, outcomes remain poor for the other half, whose cancers are resistant to radiotherapy.
Professor Chalmers is part of a team of researchers from Glasgow, Newcastle, Leeds and Manchester leading the UK-wide clinical trial. Using the funding from Cancer Research UK, which was awarded before the COVID-19 pandemic, the team hopes that the new drugs will work to make radiotherapy more effective, increase its ability to eradicate tumour cells and potentially offer new hope to lung cancer patients.
Radiotherapy kills cancer cells by damaging their DNA. Human cells have developed lots of different methods of detecting and repairing damaged DNA, and many cancers are able to use these methods to survive a course of radiotherapy.
In recent years, however, scientists have developed a number of different drugs that interfere with these methods of DNA repair. These drugs are often referred to as ‘DNA damage response inhibitors’, or DDRi.
Professor Chalmers, who is Co-Investigator on the trial, has been working with DDRi and radiotherapy for many years. He said: “We know that DDRi make lung cancer cells much more sensitive to radiotherapy in the laboratory, but we don’t know which of these drugs will be the most effective in patients with lung cancer.
“In the CONCORDE trial we will be able to test several of the most promising DDRi, and find out which have potential to improve outcomes for lung cancer patients, and which might cause additional side effects.”
A nationwide network will start recruiting patients to the CONCORDE trial in December, led by Chief Investigators Dr Alastair Greystoke at Newcastle University, Professor Corinne Faivre-Finn at The University of Manchester, co-ordinated by Leeds Cancer Research UK Clinical Trials Unit and sponsored by the University of Leeds.
Dr Alastair Greystoke, who is the Chief Investigator of the trial and as such has overall responsibility, called the work “a huge breakthrough in terms of what might be possible for future treatments”.
He said: “CONCORDE is a first of its kind multi-arm study that has been four years in the making. This trial will be at the forefront of drug-radiotherapy combination clinical trials and has the potential to transform the care for patients with lung cancer.
“This investment from Cancer Research UK enables this work to happen and drives our ideas forward. Without funding like this we couldn’t make advances both in developing new treatments and learning how to reduce side-effects from therapy.
“We are also grateful to the support of AstraZeneca who we have signed agreements to test two of their medicines, with potentially more to follow.”
The CONCORDE study will enrol participants across the UK with stage 3 NSCLC who are not suitable for surgery or concurrent chemoradiotherapy (chemotherapy and radiotherapy treatment together).
Dr Alastair Greystoke added: “Many trials across the country were paused at the peak of the COVID-19 pandemic. Thankfully, many of these trials are getting back up and running, and it’s great to be able to get this new trial off the ground after four years work. The first patients will be enrolled before the end of the year.”


































